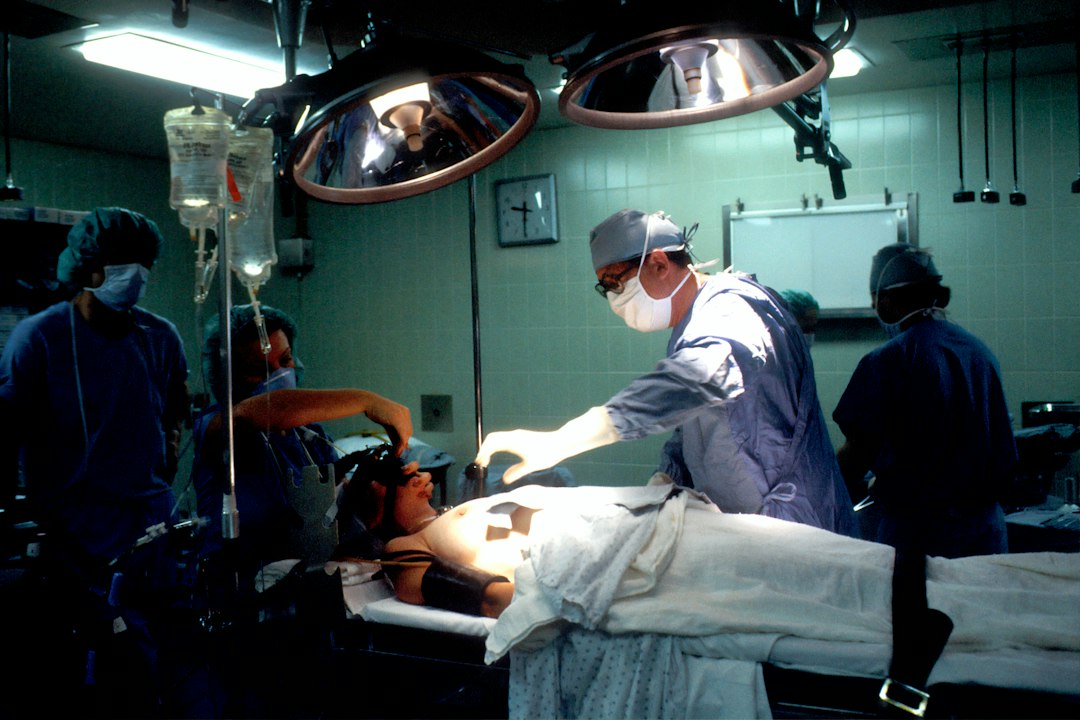
Bariatric surgery is a surgical procedure performed on individuals who are severely obese and have not been successful in losing weight through other means such as diet and exercise. The goal of bariatric surgery is to help patients achieve significant weight loss, improve their overall health, and reduce the risk of obesity-related complications. Anesthesia plays a crucial role in bariatric surgery, ensuring patient comfort and safety throughout the procedure.
In this article, we will explore the various aspects of anesthesia in bariatric surgery, including preoperative assessment and optimization, anesthetic management for laparoscopic and open surgeries, the role of neuromuscular monitoring, anesthetic techniques for morbidly obese patients, pharmacological considerations, postoperative pain management, complications and their management, and future directions in anesthesia for bariatric surgery.
Key Takeaways
- Bariatric surgery is a weight loss surgery that requires specialized anesthesia management.
- Preoperative assessment and optimization of bariatric surgery patients is crucial for successful outcomes.
- Laparoscopic bariatric surgery requires careful anesthetic management to prevent complications.
- Open bariatric surgery presents unique challenges for anesthesia providers.
- Neuromuscular monitoring plays an important role in ensuring safe anesthesia for bariatric surgery patients.
Preoperative Assessment and Optimization of Bariatric Surgery Patients
Preoperative assessment is essential in identifying any potential risks or complications that may arise during or after bariatric surgery. It involves a thorough medical history and physical examination to evaluate the patient’s overall health status. This includes assessing comorbidities such as diabetes, hypertension, sleep apnea, and cardiovascular disease.
Laboratory tests and imaging studies are also performed to assess organ function and identify any underlying conditions that may affect anesthesia or surgical outcomes. These may include blood tests to evaluate liver and kidney function, electrocardiogram (ECG) to assess cardiac health, and imaging studies such as chest X-ray or ultrasound to evaluate the anatomy of the abdomen.
Optimization of comorbidities is an important aspect of preoperative assessment. This may involve medication adjustments or initiation of new medications to manage chronic conditions such as diabetes or hypertension. It may also involve lifestyle modifications such as weight loss or smoking cessation to reduce the risk of complications during surgery.
Anesthetic Management for Laparoscopic Bariatric Surgery
Laparoscopic bariatric surgery has become the preferred approach for many patients due to its minimally invasive nature and shorter recovery time. Anesthetic considerations for laparoscopic surgery include ensuring patient comfort, maintaining hemodynamic stability, and providing adequate muscle relaxation for optimal surgical conditions.
The use of neuromuscular blocking agents (NMBAs) is common in laparoscopic bariatric surgery to facilitate surgical access and improve surgical conditions. However, the choice and dosage of NMBAs should be carefully considered to avoid prolonged paralysis or inadequate muscle relaxation.
Monitoring techniques such as end-tidal carbon dioxide (ETCO2) monitoring, invasive arterial blood pressure monitoring, and pulse oximetry are essential in ensuring patient safety during laparoscopic bariatric surgery. ETCO2 monitoring helps assess the adequacy of ventilation, while invasive arterial blood pressure monitoring allows for accurate measurement of blood pressure. Pulse oximetry monitors oxygen saturation levels in the blood.
Anesthetic Considerations for Open Bariatric Surgery
| Anesthetic Considerations for Open Bariatric Surgery |
|---|
| Preoperative evaluation of airway and pulmonary function |
| Selection of appropriate anesthetic agents and techniques |
| Monitoring of hemodynamic stability and fluid balance |
| Management of postoperative pain and nausea |
| Prevention and treatment of thromboembolic events |
| Assessment and management of comorbidities |
| Coordination with surgical team for optimal patient outcomes |
While laparoscopic bariatric surgery is the preferred approach, there are instances where open surgery may be necessary. This may be due to anatomical factors or complications encountered during the laparoscopic procedure. Anesthetic considerations for open bariatric surgery include ensuring patient comfort, maintaining hemodynamic stability, and providing adequate pain control.
Hemodynamic management is crucial during open bariatric surgery to maintain stable blood pressure and perfusion to vital organs. This may involve the use of intravenous fluids, vasoactive medications, or blood transfusions as needed.
Epidural anesthesia may be used in open bariatric surgery to provide effective pain control during and after the procedure. Epidural anesthesia involves the placement of a catheter in the epidural space, allowing for continuous administration of local anesthetics or opioids to provide pain relief.
The Role of Neuromuscular Monitoring in Bariatric Surgery Anesthesia
Neuromuscular monitoring plays a crucial role in bariatric surgery anesthesia to ensure optimal muscle relaxation and prevent complications such as residual paralysis. Neuromuscular monitoring devices measure the response of the muscles to neuromuscular blocking agents, allowing for accurate dosing and assessment of recovery.
There are various types of neuromuscular monitoring devices available, including acceleromyography, electromyography, and mechanomyography. These devices provide real-time feedback on the degree of muscle relaxation and help guide the administration of NMBAs and their reversal agents.
The benefits of neuromuscular monitoring in bariatric surgery anesthesia include improved patient safety, reduced risk of complications such as postoperative respiratory events, and improved surgical conditions. It allows for individualized dosing of NMBAs based on the patient’s response, reducing the risk of under or over-dosing.
Anesthetic Techniques for Morbidly Obese Patients
![]()
Anesthesia in morbidly obese patients presents unique challenges due to anatomical and physiological differences. Airway management can be particularly challenging in these patients due to limited neck mobility, excess adipose tissue in the upper airway, and increased risk of obstructive sleep apnea.
Various airway management techniques can be used in morbidly obese patients, including video laryngoscopy, fiberoptic intubation, and supraglottic airway devices. These techniques allow for better visualization of the airway and facilitate successful intubation.
Positioning considerations are also important in morbidly obese patients to ensure optimal surgical access and prevent complications such as pressure injuries or nerve damage. The use of specialized positioning equipment and padding can help distribute weight evenly and reduce the risk of complications.
Regional anesthesia techniques such as epidural or spinal anesthesia may be preferred in morbidly obese patients due to their potential benefits in terms of pain control and reduced risk of complications such as deep vein thrombosis or pulmonary embolism.
Pharmacological Considerations for Anesthesia in Bariatric Surgery
Pharmacological considerations are important in anesthesia for bariatric surgery due to the altered pharmacokinetics and pharmacodynamics in obese patients. Drug selection should take into account factors such as lipophilicity, volume of distribution, and protein binding.
Dosage adjustments may be necessary for certain medications in obese patients to achieve optimal drug levels. This is particularly important for medications with a narrow therapeutic index or those that are renally eliminated.
Potential drug interactions should also be considered in anesthesia for bariatric surgery. Obese patients may be taking multiple medications for comorbidities, and these medications may interact with anesthetic agents, leading to adverse effects or altered drug metabolism.
The use of multimodal analgesia, which involves the administration of multiple analgesic agents with different mechanisms of action, can help improve pain control and reduce the need for opioids in bariatric surgery patients. This can help minimize opioid-related side effects such as respiratory depression and nausea.
Postoperative Pain Management in Bariatric Surgery Patients
Effective postoperative pain management is crucial in bariatric surgery patients to ensure patient comfort, facilitate early mobilization, and reduce the risk of complications such as deep vein thrombosis or pneumonia. Various types of analgesics can be used, including opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), and acetaminophen.
Patient-controlled analgesia (PCA) is commonly used in bariatric surgery patients to allow them to self-administer pain medication within predetermined limits. This allows for individualized pain control and reduces the need for frequent nurse-administered medications.
Non-pharmacological pain management techniques such as relaxation exercises, distraction techniques, and physical therapy can also be beneficial in bariatric surgery patients. These techniques can help reduce pain perception and improve overall patient satisfaction.
Complications and Management of Anesthesia in Bariatric Surgery
Complications can arise during or after anesthesia in bariatric surgery, and it is important for the anesthesia team to be prepared to identify and manage these complications promptly. Potential complications include respiratory events such as airway obstruction or hypoventilation, cardiovascular events such as hypotension or arrhythmias, and neurologic events such as nerve injuries or stroke.
Prevention of complications involves careful patient selection, optimization of comorbidities, and adherence to best practices in anesthesia. Communication between the anesthesia team and the surgical team is crucial in ensuring a coordinated approach to patient care and prompt management of any complications that may arise.
Future Directions in Anesthesia for Bariatric Surgery
Advancements in anesthesia technology continue to improve patient outcomes and safety in bariatric surgery. This includes the development of new monitoring devices, improved airway management techniques, and enhanced drug delivery systems.
The use of personalized medicine in anesthesia for bariatric surgery holds promise in optimizing drug selection and dosing based on individual patient characteristics. This can help reduce the risk of adverse drug reactions and improve patient outcomes.
The potential for enhanced recovery after surgery (ERAS) protocols in bariatric surgery anesthesia is an area of ongoing research. ERAS protocols involve a multidisciplinary approach to patient care, including preoperative optimization, standardized perioperative care pathways, and early mobilization. These protocols have been shown to improve patient outcomes, reduce hospital length of stay, and enhance patient satisfaction.
In conclusion, anesthesia plays a crucial role in bariatric surgery by ensuring patient comfort and safety throughout the procedure. Preoperative assessment and optimization, anesthetic management for laparoscopic and open surgeries, neuromuscular monitoring, anesthetic techniques for morbidly obese patients, pharmacological considerations, postoperative pain management, complications and their management, and future directions in anesthesia for bariatric surgery are all important aspects to consider. By staying up to date with advancements in anesthesia technology and adopting a personalized approach to patient care, anesthesia providers can continue to improve outcomes for bariatric surgery patients.
FAQs
What is bariatric surgery?
Bariatric surgery is a surgical procedure performed on people who are obese, with the aim of reducing their weight and improving their overall health.
What types of bariatric surgery are there?
There are several types of bariatric surgery, including gastric bypass, sleeve gastrectomy, adjustable gastric banding, and biliopancreatic diversion with duodenal switch.
Why is anesthesia necessary for bariatric surgery?
Anesthesia is necessary for bariatric surgery to ensure that the patient is comfortable and pain-free during the procedure. It also allows the surgeon to perform the surgery safely and effectively.
What types of anesthesia are used for bariatric surgery?
The most common types of anesthesia used for bariatric surgery are general anesthesia and regional anesthesia. General anesthesia involves putting the patient to sleep, while regional anesthesia involves numbing a specific area of the body.
What are the risks of anesthesia for bariatric surgery?
The risks of anesthesia for bariatric surgery include allergic reactions, breathing problems, and blood pressure changes. However, these risks are generally low and can be managed by an experienced anesthesia team.
How long does the anesthesia last for bariatric surgery?
The duration of anesthesia for bariatric surgery depends on the type of surgery and the patient’s individual needs. However, most bariatric surgeries take between 2-4 hours, and the anesthesia typically lasts for the duration of the surgery.
What should I expect after anesthesia for bariatric surgery?
After anesthesia for bariatric surgery, patients may experience some side effects such as nausea, vomiting, and dizziness. However, these side effects are usually temporary and can be managed with medication and rest. Patients will also be closely monitored by the anesthesia team and nursing staff to ensure a safe and comfortable recovery.